Rejuvenating and regenerating the skin with biodegradable polymers
A person’s skin can often give an indication of their overall well-being and health. Biomaterial technologies used for treating wounds, scars and to counteract skin aging have progressed rapidly in recent years. Moreover, consumers and patients are increasingly interested in finding sustainable, less invasive solutions for regenerating their skin. As the main structural protein family in the body, collagen enables the skin to self-heal after injury or damage and can counteract the aging process.
Collagen makes up between a quarter and a third of the total protein mass in humans and other animals. It is completely biodegradable and has a high degree of biocompatibility, making it ideal to support tissue repair. In therapeutic applications, collagen can be processed into the desired form and applied directly to the skin. Collagen can also be rebuilt by the body’s own cells and the body can be stimulated to produce its own collagen, for example, in the skin.
This article examines two aspects of sustainable skin self-healing: the use of non-animal-derived collagen for tissue regeneration, and the use of bioresorbable polymer powders to stimulate the body’s natural collagen production.
1. Non-animal-derived collagen for tissue regeneration and wound healing
More than 28 types of collagen have been identified to date, each with specific properties such as rigidity, shape, and integrity. These collagen types are critical to the formation and functionality of various parts of the body including tissues, skin, cartilage, organs, bone, bone marrow, cell membranes, ligaments, hair, and the lungs. Because of its well-defined structure and interaction with cells and tissues, collagen has a wide range of applications. It can be processed directly, or in some cases using additional chemical modification technologies, into a variety of forms such as lyophilized powders, liquid solutions, hydrogels, films or meshes and sponges for use in a wide variety of health care applications.
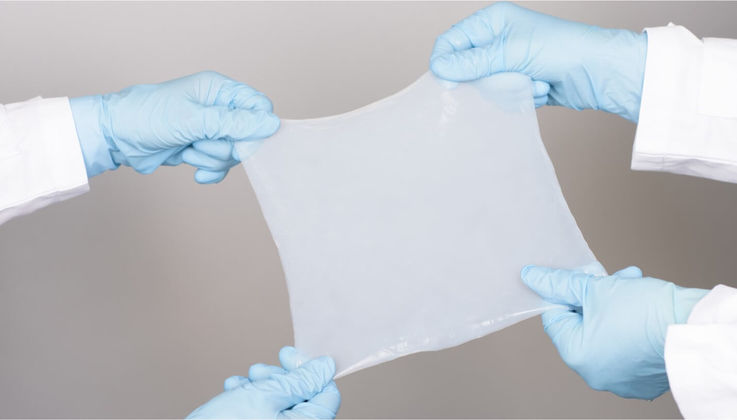
Collagen is widely used in a number of common orthopedic, cardiovascular, ocular, general surgical, dental, regenerative medicine and wound care applications. In burn and wound healing, collagen can be applied as a wound dressing or temporary skin replacement to stimulate the growth of new tissue. The dressings are used in direct contact with the wound bed, absorbing discharged matter and hydrating the skin to promote healing. Chronic wounds are characterized by persistent inflammation, destruction of the extracellular matrix (ECM) and lack of active soluble mediators in the wound healing process. Collagen dressings help to stimulate these processes and can therefore accelerate the healing of chronic wounds.
Non-animal derived collagen
Almost all medical and pharmaceutical grade collagen used today is derived from animal sources, such as the skin or tendons of cows and pigs. Some collagen is also extracted from marine sources such as fish or jellyfish. For a limited number of R&D activities, collagen is also extracted in very small quantities from the human placenta after the birth of a child.
The supply of collagen from traditional animal sources has several risks related to safety, consistent reproducibility, sustainability, and consumer acceptance. There is a risk of pathogen and disease transmission, immunogenic or allergic reaction, as well as the issue of sustainability, as the harvesting of collagen from animals has a significant impact on the environment. Furthermore, many people choose not to consume or use animal products for ethical or religious reasons.
Quality and reproducibility
For many medical and pharmaceutical applications, including wound care, it is critical that collagen can be made using a process that ensures its properties and characteristics are reproducible to enable consistent interaction with cells and tissues. The industrial process to extract, sterilize, purify, and deliver traditional sources of collagen in a reproducible manner is extremely challenging and costly. Many healthcare companies and regulatory agencies would prefer a source of collagen that provides batch-to-batch reproducibility.
Evonik’s non-animal-derived collagen
Evonik has developed a unique collagen platform technology that can address unmet market needs for the use of collagen in healthcare and other life science applications. The technology is devoid of all animal and human origin materials and features a triple helix structure that enables it to mimic (and in some cases potentially enhance) the properties of natural collagen.
This recombinant collagen is also designed to be highly soluble at physiological pH, making it suitable for enhanced cell interaction and adhesion. It is also designed to be used with various cross-linking and technologies so that it can be processed into a variety of forms and shapes such as gels, powders, creams, foams, fleece, and sponges, making it especially suitable for wound healing.
The fermentation-based process takes place under precisely defined conditions to enable the production of collagen with a high degree of purity that is reproducible at development or commercial scale. This consistent level of reproducibility and efficient scalability is difficult to achieve with other known collagen sources.
In addition to producing and supplying collagen in a variety of forms, Evonik also leverages its global application, formulation and manufacturing expertise with biomaterials, drug products and tissue engineering to support customers in the development and commercialization of their own products. These services complement Evonik’s existing core competencies in the development and supply of biomaterials and drug products, as well as the production of active pharmaceutical ingredients, advanced foods, and bio-fabricated materials through fermentation-based processes.
2. Bioresorbable polymer powders used in dermal fillers
As we age, the face loses fat and volume while the skin loses collagen and elasticity. Dermal fillers, also known as soft tissue fillers, are injected under the skin using a minimally invasive procedure to plump thin lips, enhance shallow contours, soften facial lines, remove wrinkles, and improve the appearance of scars. Unlike Botox – another popular minimally invasive procedure –dermal fillers do not freeze muscles using purified bacteria, but rather contain ingredients that add fullness to areas that have thinned due to aging.
Dermal fillers help restore volume and augment soft tissue, and are often used as an effective complement to facial surgery. The quick procedure produces reliable results and minimal downtime for the patient.
Materials used in dermal fillers
Dermal fillers can be based on several different materials, including hyaluronic acid, collagen, and bioresorbable polymers such as Poly-L-Lactic acid (PLLA) or polycaprolactone (PCL). Although collagen fillers can be injected directly under the skin to replace the skin’s natural collagen, the effect is not as long-lasting as other fillers and there may be adverse or allergic reactions.
Suitable alternatives are PLLA or PCL, which Evonik markets for use in dermal fillers as part of its RESOMER® portfolio of bioresorbable polymers. Both are biodegradable, biocompatible, synthetic polymers that are widely used in implantable medical applications such as absorbable sutures and bone screws. When used in fillers, they are particularly long-lasting and are administered in a series of injections over a period of several months. The effects of bioresorbable polymers generally become increasingly apparent over time – typically several weeks – and last for up to two years.
Advantages of bioresorbable polymer-based fillers
Polylactic acid-based dermal fillers are a semi-permanent correction procedure that stimulate the body to produce its own collagen. The key benefit of these fillers over other dermal fillers, such as those based on hyaluronic acid, is their long-lasting effect. After initial treatment with PLLA- or PCL-based fillers, the result improves over time as the dermal thickness expands, and the positive effects can be seen for up to two years (hyaluronic acid effects typically last one year). They are fully biodegradable as they metabolize to water and CO2 over time.
Powders for dermal filling
The well-established RESOMER® polymers can be converted into a fine powder for use in dermal fillers. With a 30-year track record for efficacy, safety, biocompatibility and supply security, these polymers have been widely used in medical device applications such as for wound healing, orthopedic devices, and cardiovascular devices. By disintegrating RESOMER® pellets into a GMP-grade bioresorbable powder, RESOMER® can be successfully used in dermal fillers. Evonik has developed a unique solvent-free technology to reduce the particle size of high molecular weight polymers for use in dermal filler applications. This powder technology requires no solvent and is compatible with a range of polymers suitable for dermal fillers including PLLA. The particle size distribution is tunable in a range of less than 100 micrometers. These powders also meet high quality standards: they are manufactured in ISO Class 8 clean rooms, ISO 13485 and GMP compliant, and are suitable for human use.
Interested in learning more?
For further information about non-animal-derived recombinant collagen or the RESOMER® powders for dermal fillers, or to request a sample of these products, please get in touch with Caroline Lauret: caroline.lauret@evonik.com or visit our website here:
https://healthcare.evonik.com/en/medical-devices
Visit and register for Evonik’s Health Care platform onCare to find out about our latest products, download support material, register for webinars and chat directly with our experts:
https://oncare.evonik.com/